CANCER OF UNKNOWN PRIMARY FOUNDATION
The basics of cancer
Cells and cancer
To begin to understand Cancer of Unknown Primary (CUP) one needs to understand first a bit about how cancer starts, and that involves our cells: the human body is composed of billions of cells. Cells are the clever little building blocks that make up the organs and tissues of our bodies.
Our cells are genetically programmed to do various things throughout our lifetime. We need new cells to replace worn out cells that die in a regular cycle. If (the DNA in) a cell becomes faulty, cells can start growing uncontrollably and form a tumour – a ‘swelling’ but in the cancer context the word is used to denote abnormal growth of tissue.
If the tumour is abnormal it is known as ‘malignant’; if it is not cancerous it is known as ‘benign’. The word ‘lesion’ is sometimes used. Lesions are caused by any process that damages tissues. A cancerous tumour is an example of a lesion. A benign tumour does not spread within the body; but an untreated, malignant tumour is likely to spread (metastasise).
Early diagnosis is important. However, a tumour may not be apparent and the symptoms may not be recognised by the patient or the doctor.
Causes of cancer
Cancer is a genetic disease. It is caused by a number of changes (mutations) in the genes in our body that control cell growth or regulate the detection and repair of DNA damage. Often there is more than one gene involved in cancer development.
Cancer is the result of accumulated mutations to a person’s DNA. The mutations that can lead to cancer may be inherited or acquired. Multiple events have to occur to cells before cancer occurs (which is why few children get cancer, unless it is through inherited damage, and why those over 60 are more likely to get cancer).
Mutations may result through a loss of activity in Tumour Suppressor Genes (the brakes), or enhanced activity by Oncogenes (accelerators), that regulate the way our cells work. So, whilst we may have a genetic predisposition to a particular cancer it needs further ‘hits’ to turn this into cancer. The damage, or additional damage, can be caused by a wide variety of factors such as: lifestyle (diet, drink, smoking, sunbathing etc.), radiation exposure, stress, viral infection, chemicals.
The primary
The point of origin in the body, where the genes have caused cells to grow uncontrollably and form a tumour, is known as the primary site. In most cases the primary site is obvious and quickly diagnosed. Conventional medical wisdom suggests the importance of finding the primary; but as diagnosis and medicines get increasingly personalised (e.g. through genomic profiling for CUP) it will become a case of: what is the pattern of this disease we need to define a treatment for, rather than where is the primary site?
Strictly speaking CUP exists from the point someone presents with metastatic cancer without an obvious primary site until they know for certain the site of the primary. Following the NICE Guideline for CUP (2010) when the initial diagnosis is uncertain this is described as MUO or metastatic malignancy of unknown primary origin. It becomes CUP when it remains impossible to tell, from increasingly sophisticated tests (X-rays, blood tests, scans etc.), where the cancer began in the body.
Metastasis
Metastasis means the spread of cancer. This spread is common to many cancer patients by the time they see their doctor and, although it means that surgery is unlikely to be the main treatment, the cancer remains treatable.
Cancer cells that break away from a primary tumour are carried around the body by the bloodstream or the lymphatic system. The cells that escape from a primary site and form a secondary site or sites are known as secondary cancers or metastases. Metastasis is the process and this is easy to understand if one goes back to the Greek origins of the word. Literally it means going beyond (meta) standing still (stasis).
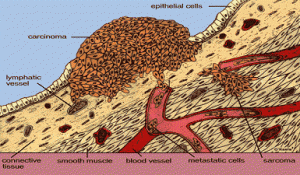
Source: www.cancerinfo.com
Metastatic cancer is sometimes evident in visible lumps (lesions) and in images captured by X-ray, PET-CT and similar techniques.
Every tumour is different and every ‘host’, i.e. the patient, is different. The genetic make-up of people probably has something to do with their vulnerability to the cancer spread. Using specialized diagnostic tests and microscopes, a pathologist tries to tell where the cancer cells came from. Usually, cancer cells look like abnormal versions of cells in the tissue where the cancer began but the visible and chemical clues are not always apparent with CUP; CUP seems to behave differently to other cancers in a way that is not yet understood.
Where these loose cancer cells choose to lodge is random, but these cells form a new, or secondary, tumour. There is a ‘seed and soil’ theory that the metastatic cells (cancer seed) from an identified primary colonise particular organs (the soil). This does not seem to be the case with CUP where metastasis is unusual (atypical); making it more difficult to work backwards in terms of the diagnosis from the secondary sites with any confidence.
The cells in the metastatic tumour are genetically those of the original tumour. This means, for example, that if breast cancer spreads to the lungs, the metastatic tumour in the lung is made up of cancerous breast cells (not lung cells) and this is then described as metastatic breast cancer (not lung cancer). Chemotherapy drugs are designed to target the primary, or ancestral, cancer cells which is why finding the origin of the cancer is important for treatment.
Symptoms
The signs and symptoms of (metastatic) cancer are different for everyone – for some there may be no symptoms; for others there may be general physical deterioration. Some of the symptoms can include: breathlessness, discomfort in the chest, or a collection of fluid around the lungs, bone pain, back pain, swelling and discomfort in the tummy (abdomen), swollen lymph glands such as those in the neck, underarm, chest or groin (they may feel hard and swollen or cause pain through pressure on tissue or nerves nearby). Additional, generalised symptoms such as: weight loss, headaches, no appetite, feeling extremely tired are all things that your GP will want to know about. See ‘going to the GP‘.